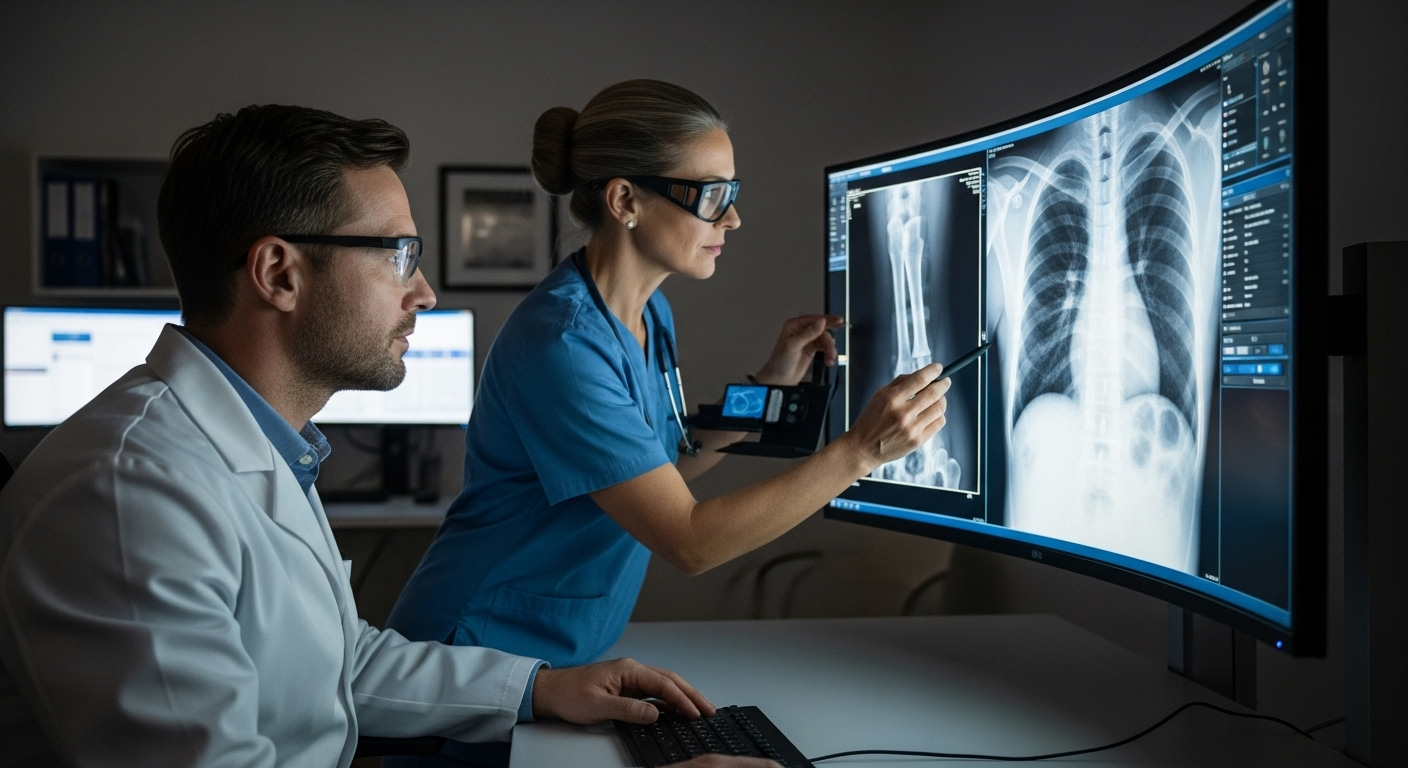
Key Takeaways
- CMS has permanently adopted virtual direct supervision for diagnostic tests, including contrast imaging, beginning January 1, 2026, making a COVID-era flexibility into lasting policy.
- Virtual supervision requires real-time, two-way audio and video communication—audio-only methods do not qualify under the new federal standard.
- Healthcare providers can expand access to care, optimize workforce deployment, and improve operational efficiency while maintaining compliance with Medicare requirements.
- Practices must implement HIPAA-compliant technology, update supervision protocols, and ensure alignment with state laws before the January 2026 implementation.
The healthcare landscape is undergoing a significant transformation as the Centers for Medicare & Medicaid Services (CMS) establishes permanent virtual supervision standards for diagnostic imaging. This landmark policy change is already reshaping how imaging centers, radiology practices, and hospitals deliver contrast-enhanced services while maintaining the highest safety standards.
CMS Finalizes Permanent Virtual Supervision Starting January 1, 2026
On October 31, 2025, CMS released the Calendar Year 2026 Medicare Physician Fee Schedule Final Rule, cementing a revolutionary shift in healthcare supervision policy. Beginning January 1, 2026, supervising physicians and non-physician practitioners can permanently meet the “presence” and “immediate availability” requirements for direct supervision through real-time, two-way audio and video communication technology.
This decision transitions what began as a temporary COVID-19 flexibility into a permanent Medicare policy feature. The change recognizes that modern telecommunication tools can effectively uphold safety, accessibility, and quality standards in clinical supervision without requiring physical presence.
The permanent adoption of virtual supervision validates the effectiveness of technology-enabled oversight models that have proven successful during the pandemic era.
What Changes in the New Direct Supervision Policy
The 2026 Final Rule fundamentally alters how direct supervision is defined and delivered across healthcare settings. Under the new policy, supervising clinicians can fulfill supervision requirements for diagnostic tests governed by 42 CFR § 410.32 through secure, interactive audiovisual platforms rather than physical presence.
Real-Time Audio-Video Technology Requirements
CMS has established strict technology standards to ensure virtual supervision maintains the same safety and responsiveness as in-person oversight. Real-time, two-way audio and video communication is mandatory—audio-only methods explicitly do not qualify under the federal standard. The technology must provide uninterrupted connectivity, enabling immediate intervention when necessary.
Healthcare providers must implement HIPAA-compliant platforms with latency monitoring and failover mechanisms. Session logging capabilities are required for audit verification and documentation requirements. The technology should support clear visual assessment of patient conditions and seamless communication between supervising physicians and on-site staff.
Office-Based Settings and IDTF Coverage
The virtual supervision flexibility applies across office-based practices and Independent Diagnostic Testing Facilities (IDTFs). This broad coverage ensures consistent supervision standards regardless of practice setting or organizational structure.
Within IDTFs, specific qualifications apply: only physicians with demonstrated proficiency in performing and interpreting the supervised test may provide remote oversight. This requirement ensures that virtual supervisors possess the clinical knowledge necessary to guide procedures and respond to complications effectively.
Excluded Services Still Require In-Person Oversight
CMS has maintained safety-based exclusions for high-risk procedures. Services with 010 (minor, 10-day global) or 090 (major, 90-day global) surgical indicators remain excluded from virtual supervision eligibility. These procedures require on-site physician availability due to their inherent procedural risks and potential for immediate complications requiring rapid intervention.
This balanced approach ensures that virtual supervision improves operational efficiency without compromising patient safety in scenarios where physical presence remains clinically required.
Benefits for Healthcare Providers and Patient Access
The permanent adoption of virtual direct supervision delivers transformative advantages for healthcare delivery, addressing longstanding challenges in access, efficiency, and workforce management.
1. Expanded Access in Rural and Underserved Areas
Rural healthcare facilities and underserved communities often struggle to recruit and retain on-site radiologists. Virtual supervision eliminates geographic barriers, allowing facilities to schedule diagnostic procedures without requiring a supervising physician to be physically present. This breakthrough reduces patient travel distances, minimizes appointment delays, and ensures consistent access to contrast-enhanced imaging services.
Healthcare systems can now provide specialized oversight to remote locations, bridging critical gaps in specialist coverage that have historically limited access to advanced diagnostic services.
2. Improved Operational Efficiency and Scheduling
Virtual supervision transforms operational workflows by enabling extended service hours and improved resource utilization. Imaging centers can now offer early morning, evening, and weekend services without compromising compliance or safety standards. This flexibility eliminates the costly delays and cancellations that occur when on-site supervision is unavailable.
Scheduling benefits include:
- Reduced exam cancellations due to supervision gaps
- Improved scanner utilization rates
- Better patient throughput
- Lower operational overhead costs
3. Optimized Specialist Workforce Deployment
The policy enables more efficient use of scarce radiologist resources. Supervising physicians can oversee multiple locations simultaneously, reducing non-clinical travel time and maximizing clinical productivity. This optimization is particularly valuable given ongoing radiologist shortages and increasing imaging demand.
Healthcare systems can deploy specialists more strategically, concentrating knowledge where it’s most needed while maintaining supervision coverage across their entire network. This approach reduces physician burnout while expanding service capacity.
Compliance Requirements and Implementation Steps
Successfully implementing virtual supervision requires careful attention to regulatory compliance and operational preparation. Healthcare providers must address technology infrastructure, documentation protocols, and regulatory alignment to ensure smooth transitions.
Technology Standards and Documentation
CMS compliance demands strong technology platforms that meet specific performance criteria. Required technology features include:
- HIPAA-compliant secure communication channels
- Real-time audiovisual connectivity with minimal latency
- Automated session recording and audit trails
- Emergency escalation and backup communication systems
Documentation requirements are equally critical. Facilities must maintain contemporaneous records detailing supervising clinician credentials, participation times, technical interruptions, and corrective measures. Patient consent and acknowledgment of virtual oversight must be properly documented and readily available for audits.
State Law and Professional Guidelines Alignment
While CMS establishes federal standards, state laws may impose additional requirements or limitations on virtual supervision. Healthcare providers must carefully review applicable state regulations, particularly concerning contrast media administration and adverse reaction management.
Professional guidance from organizations like the American College of Radiology (ACR) provides a framework for safe virtual supervision practices. These guidelines address contrast injection protocols, the technologist’s scope of practice, and emergency response procedures that complement CMS regulations.
How This Policy Addresses Healthcare Industry Challenges
The permanent virtual supervision policy represents CMS’s strategic response to systemic healthcare challenges that have intensified in recent years.
Solving Radiologist Shortage Issues
According to the Association of American Medical Colleges, the U.S. faces a projected shortfall of over 20,000 radiologists by 2034, with imaging demand continuing to outpace specialist supply. This shortage creates bottlenecks in diagnostic imaging, leading to delayed diagnoses and compromised patient care. Virtual supervision directly addresses this challenge by enabling existing radiologists to provide oversight across multiple facilities simultaneously.
The policy allows healthcare systems to optimize their specialist workforce without geographical constraints. A single radiologist can supervise contrast procedures at several locations throughout a day, maximizing their clinical impact while maintaining safety standards. This efficiency gain is vital for addressing the growing demand for diagnostic imaging services.
Modernizing COVID-Era Temporary Flexibility
During the COVID-19 pandemic, CMS implemented temporary virtual supervision flexibilities that proved both safe and effective. The healthcare industry adapted quickly to these changes, developing strong protocols and technology solutions for remote oversight. The permanent policy codifies these successful innovations, providing regulatory certainty for long-term planning and investment.
This transition from temporary to permanent policy reflects CMS’s confidence in virtual supervision models and recognition that technology-enabled oversight can improve rather than compromise patient care quality.
Implementing Virtual Supervision: What Your Practice Needs to Get Right
With the January 2026 rule now in effect, practices that haven’t yet adopted compliant virtual supervision workflows need to move quickly. Getting it right requires systematic planning, technology assessment, and staff training.
Implementation priorities include:
- Evaluating current technology infrastructure and identifying upgrade requirements
- Developing virtual supervision protocols and emergency response procedures
- Training staff on new workflows and communication systems
- Updating documentation templates and audit preparation materials
- Reviewing state regulations and professional guidelines for additional requirements
Early preparation enables practices to capitalize on virtual supervision benefits while avoiding compliance risks. Organizations that begin implementation planning now will be better positioned to take advantage of the operational advantages and expanded access opportunities that virtual supervision provides.
CMS plans to monitor outcomes through quality reporting and utilization reviews, so thorough documentation isn’t just a compliance step — it also contributes to the broader evidence base that will shape how virtual supervision evolves going forward.
ContrastConnect
Las vegas
Las Vegas
NV
89109
United States
